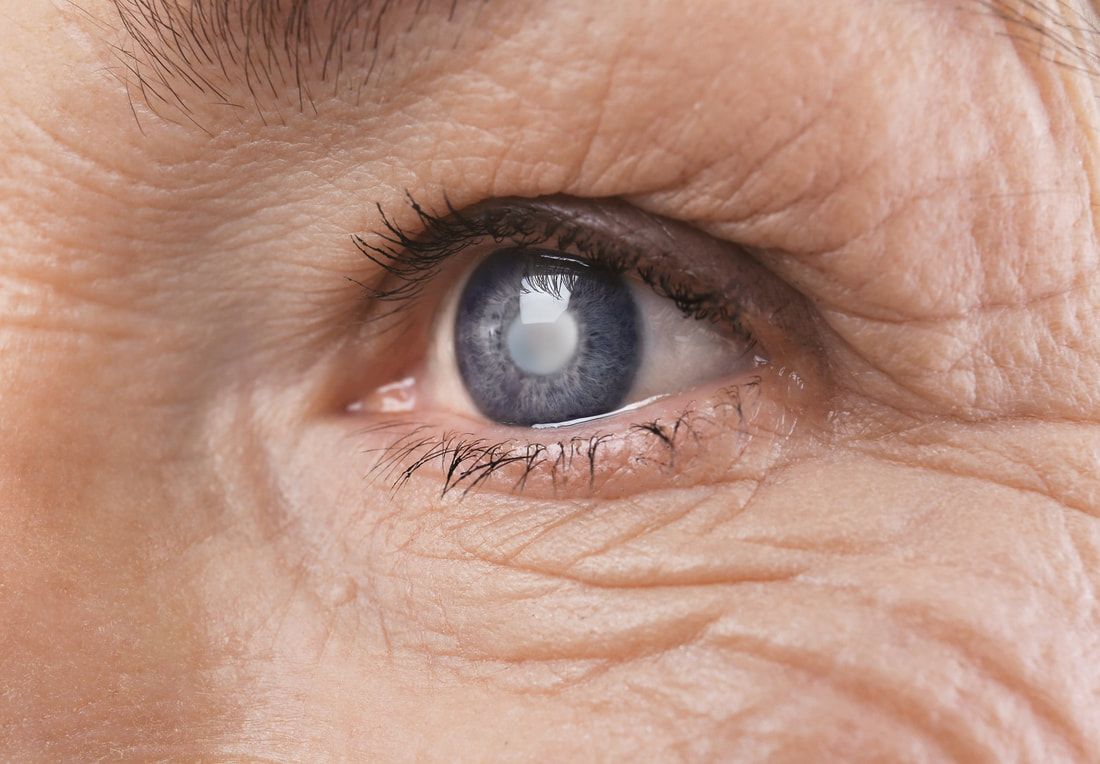
Cataracts
Historically, cataracts have been related with age related changes in the internal lens. These changes can be accelerated with accumulated UV light exposure, aging and health issues such as diabetes or high blood pressure. Fortunately, cataract surgery has come a long ways and now has the opportunity to provide patients with renewed vision. Implant technology now offers doctors the ability to correct all different types of prescriptions and in some cases even provide reading capabilities again.
Play Video
Glaucoma
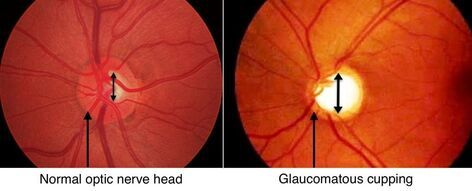
Glaucoma is termed "the silent thief of the night" mainly because of its slow subtle changes over time that can take away vision. Glaucoma is a disease where the nerve tissue in the eye deteriorates in the causing tunnel vision. Sometimes, these changes can occur due to high eye pressure.
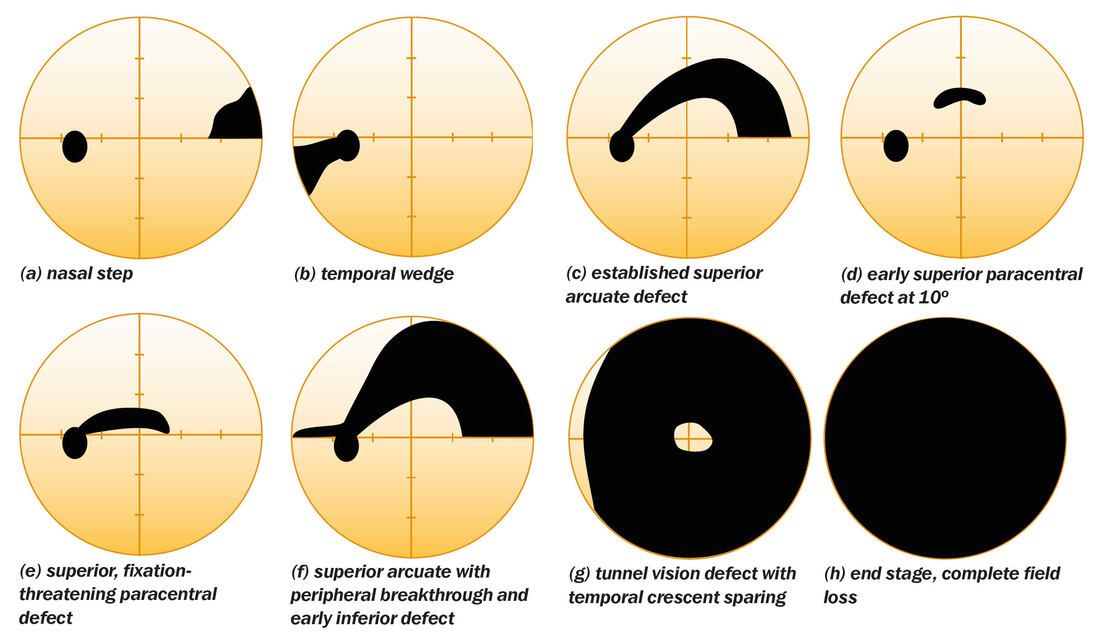
Unfortunately, it isn't until the cases are fairly advanced that patients notice the issues and unfortunately, at this point there is no way to restore lost vision. The gradual changes and the brains ability to fill gaps in the vision lead to slow detection. Testing in office is focused on identifying early stages of glaucoma including extensive peripheral vision analysis, eye pressure measurements and optic nerve head scans/analysis.
Play Video
Macular Degeneration
Another 'age-related' disease known as macular degeneration can impact central vision. Studies have shown aging and smoking are the two highest risk factors in developing this sight threatening disease. However, new research also points towards the role of genetics, cardiovascular health, poor nutritional intake and an abnormal Body Mass Index.

Dry Macular Degeneration is a slower progressing condition resulting from waste deposition in the retina due to an inability to clear metabolic waste. This waste deposition creates a toxic landfill that damages the retina and can lead to abnormal blood vessel growth beneath the retina known as Wet Macular Degeneration. These vessels can bleed and rapidly damage central vision.
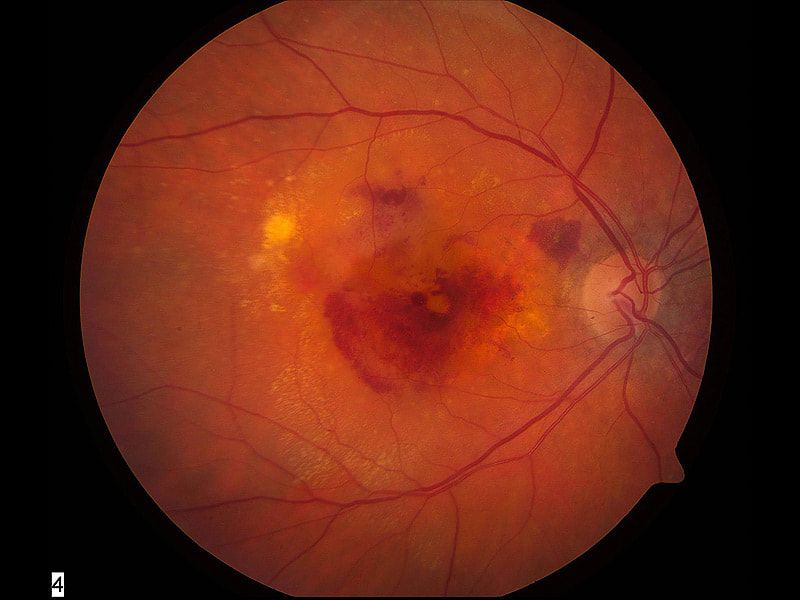
Early detection is important in modifying lifestyle behaviors to decrease risk of progression. In addition, routine visits are important to assess for conversion of dry Macular Degeneration to wet Macular Degeneration.
Play Video
Vitreous Detachment
A posterior vitreous detachment occurs when the gel filling the eye starts to separate from the internal lining or the retina. This can cause flashes of lights or floaters in the vision. Typically, this process will occur in everyone as they age, but if there are symptoms of flashes or new floaters, a small percentage of these patients can suffer from tears in the retina or neuro-sensory layer of the eye. This can potentially lead to complete vision loss if the lining separates due to a break in the wall paper.
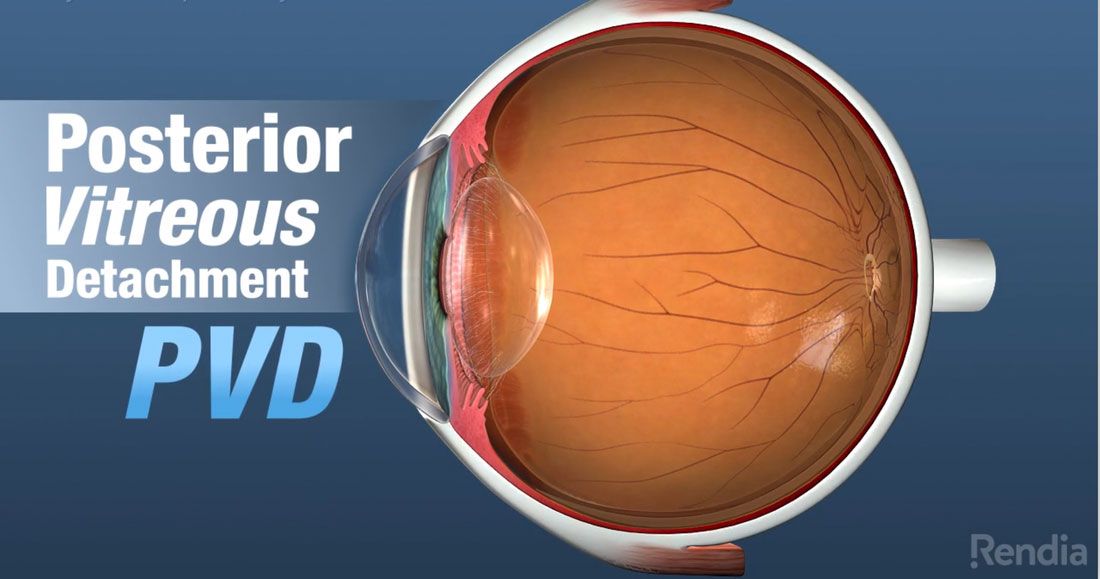
It is important to have an evaluation immediately if you experience symptoms of flashing lights, floaters or a curtain in your vision to rule out a potential retinal detachment. This process can take up to a year to complete and symptoms should be monitored closely with your doctor.
Play Video

Retinal Detachment
A retinal detachment can occur in the eye when there is a tear in the internal lining. Sometimes this can be a sudden occurrence associated with flashes of lights, floaters and followed by a curtain in your vision.

Other times, these can be fairly asymptomatic initially and picked up on a general routine examination before it is too severe. A retinal detachment can cause sudden and permanent vision loss if not treated and addressed right away. The causes of retinal detachments can include direct trauma, diabetes, systemic health issues, high levels of near-sightedness and aging changes.
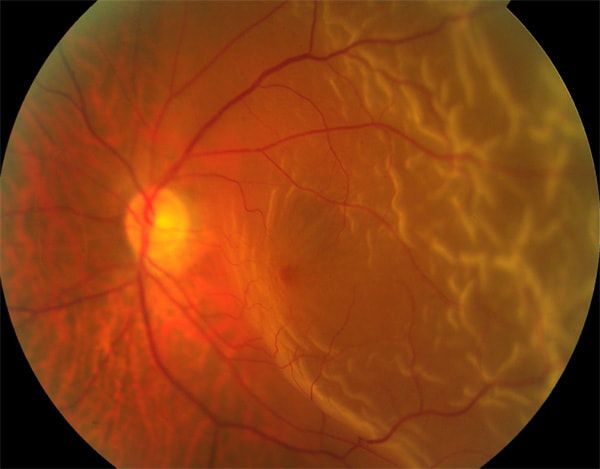
This condition can affect individuals of all ages. Fortunately, if caught early, retinal surgery has come a long ways in saving and restoring vision.
Play Video
Diabetic Retinopathy
Diabetes is a metabolic disease that impacts the way we process sugar in our bodies. This can lead to systemic issues such as increased risk of stroke, cardiovascular disease, poor wound healing. In addition to systemic complications, vision loss can also occur within the eyes leading to vision loss if blood sugar is not sufficiently controlled.
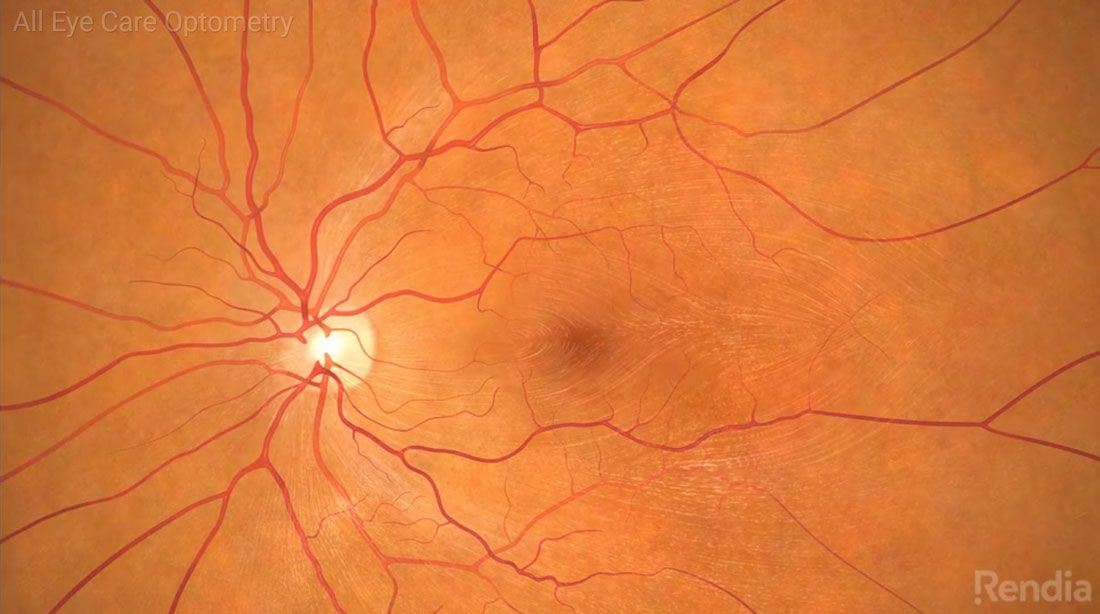
Normal Retina
Examinations are especially important in diabetics to identify potential threats to the central vision due to leaking blood vessels. Fortunately for diabetics, early detection in retinopathy and pro-active changes in lifestyle can decrease the risk of progression to vision loss.
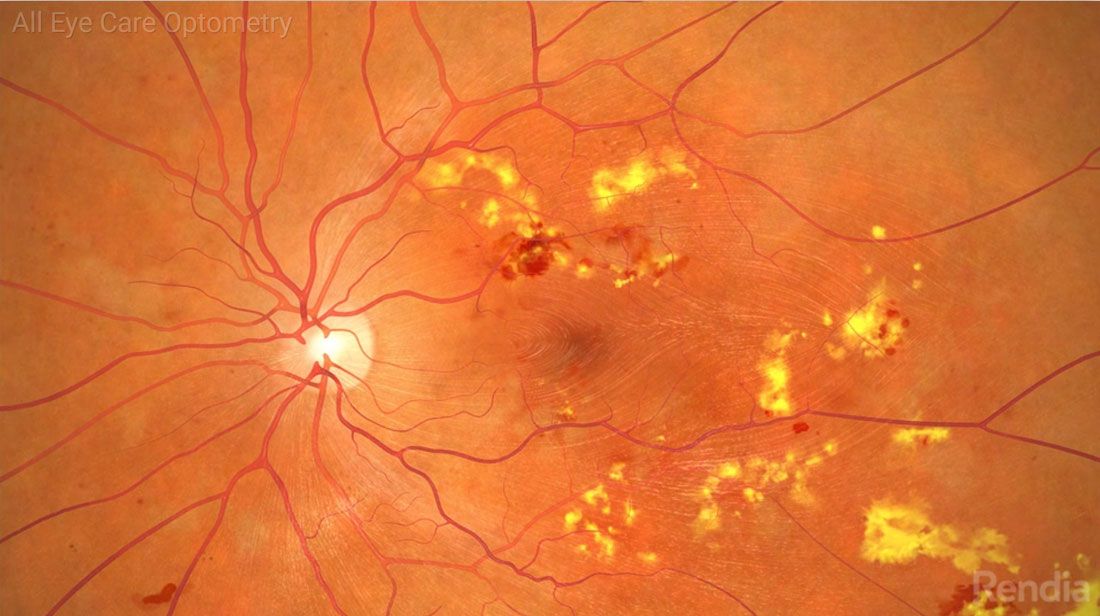
Diabetic Retinopathy
Dry Eye Disease

Dry eye disease occurs due to an inability to produce enough tears or an over evaporation of the existing tears in your eyes. This can cause significant discomfort and irritation impacting quality of life as well as causing severe disruptions in your vision. In addition to symptoms of burning, stinging, grittiness, symptoms of fluctuating vision when blinking and excess tearing can all be signs of a dry eyes. Contrary to popular belief that dry eyes is merely a nuisance, dry eyes can lead to severe complications including corneal damage and inflammation.
Play Video
Eye Diseases

With over 200 different diseases that can manifest in the eye, a routine examination is important in identifying these issues and finding the root cause. Your eye doctor will communicate with your primary care physician if additional testing is necessary to identify underlying health issues. It is surprising the level of information that can be obtained by just looking inside your eyes!